|
Startseite
|
|||
Measurement of heart beat and blood oxygen level as an aid to therapeutic diagnosis during the course of therapy The concept of a therapy-interactive diagnostic process: Simple and straightforward diagnoses are not as common in the therapy room as one would wish, and even less likely to be of much duration. Teumer took account of this fact when he referred to the need for "diagnosis to run alongside therapy on an interactive course"; this comes closer to reality in the everday work of the therapist. Every new piece of information gathered – and therapeutic intervention is bound to bring forth more information (information registered both consciously and subconsciously are known to converge in this process) – alters the therapist´s view of the problem constellation and changes the general nature of that constellation. This process could be said to remotely resemble the rotation of a kaleidoscope, which causes the tiny glass fragments inside to change position and produce a new picture, one with different patterns and combinations. Unlike the kaleidoscope, however, a therapy-interactive diagnosis also brings to light further pieces of information, adding to the already increasing number of elements. If the sheer quantity of additional information exceeds certain limits, the quality of the diagnosis will suffer; this is a proven and widely known fact. As the amount of information a therapist can process when making an initial diagnosis will invariably depend on his or her own individual capacity to do so (also confirmed by research), it is only to be expected that further information that will have a bearing on the ultimate individual diagnosis can only be obtained gradually during the course of treatment. Measurement of pulse and blood oxygen levels One diagnostic method that can be used in the therapy-interactive diagnostic process is measurement of heartbeat and blood oxygen levels using a monitoring device applied to the fingertip. Readings of heartbeat and blood oxygen level can indicate the presence of vegetative components in the patient´s interaction with his or her environment in a given situation or in a situation being talked about. Information of this kind will be extremely hard to gather by simply asking questions and looking out for such crude pointers as a pale discolouring and cooling of the extremities or facial flushing. A glassy stare or a daydreamy look could be a sign of deep reflection just as well as a reaction to a considerable fall in heart rate – something the naked eye will be unable to distinguish. The idea of using such an instrument in the therapy room came from processing data collected from a manual therapy practice (Dr. L. E. Koch, Hamburg) many years ago. The subject of that study was to monitor changes in the heart rate (HR) of babies following manual therapy treatment. In the subsequently published article (L.E. Koch, H. Koch, S. Graumann-Brunt, D. Stolle, J.R. Ramirez and K.S. Saternus: Heart rate changes in response to mild mechanical irritation of the high cervical spinal cord region in infants. Forensic Science International Volume 128, Issue 3, August 28, 2002, Pages 168 – 176), attention was directed at circumstances that might lead to SID; it was the very young babies that were the subject of concern, but observation of older babies (upwards of 4 months) delivered some additional information. With some babies heart rate began to rise, with others it fell, and in other instances it rose considerably, then fell again, only to begin rising once more. The search for some pattern, some rule or other, could not be pursued any further at the time, nor could any closer consideration be given to the possible causes of these different reactions; there was no scope for an assessment of these occurrences. Work towards an understanding of this aspect of the study did not proceed any further (as is often the case with empirical research). The unanswered questions were left for the routine of everyday therapy to deal with. But there was now an awareness that there might be some unexpected hidden processes at work "behind the scenes", as it were, in autonomous functions, which may greatly influence the way children cope with challenging situations. This is what led to the use of the instrument for measuring heart rate and blood oxygen levels for therapeutic diagnosis purposes and during the course of therapy itself. In the therapeutic practice submitting its findings in this report the measurement of heart rate and blood oxygen level has since become an indispensible and highly informative everyday aid to diagnosis and therapy, not only of children, but of adult patients as well. It goes without saying that one should always beware of the danger of over-interpreting results obtained in this way. It is of utmost importance to remember that we are dealing with indicators that may be inaccurate. As it is in no way obtrusive, however, the sensor can be left on the fingertip a while longer, thus enabling the therapist to observe reactions en passant and to gather information for subsequent screening. The instrument is also useful when doing exercises to engage the muscles of the abdomen to properly initiate the pronunciation of the "sh" (German "sch") sound, for example, or when working on abdominal breathing; patients have been quite keen to use it because they can then see for themselves what effects their efforts are having. Here, to illustrate the point, are just some of the more notable phenomena where a recording of HR proved most helpful; quite considerable decreases were observed - when the patient was asked to perform a particular task or to contemplate the task in question, - when the patient had difficulty doing arithmetic, - where under-performance was accompanied by digestive disorders, - when switching the field of vision (a variety of different circumstances and problems, e.g. often noticed where a patient was learning to read), - when being spoken to by strangers, but also by (close or other) relatives or persons known to them (more common among children, but also occurring among prematurely-born adults), - where a patient had scars or some skin peculiarity ( quite different in nature, in one particular case due to exposure to drip infusion apparatus as a baby, but also skin flaps, etc.) - when hands or feet are touched ( two instances of note where births had been Caesarean sections), - at the mention of swimming lessons at the indoor swimming baths during school time (e.g. a patient in one case having already undergone SID resuscitation – a drastic decrease in HR), - when the position of the patient´s body was changed (very severe and protracted e.g. in the case of one child with Louis Bar syndrome), In each of the examples listed below the measures compiled for each individual case were carried out with continued use of the appliance to monitor progress. - exercises practised in neurophysiological development therapy, but also simple exercises done with the eyes closed, work done on focussing visual attention with eyes open and closed, work done with vertical lines (using the force of gravity for orientation) with eye training but also drawing exercises, straightening up exercises, mobilization of the nape of the neck (alertness), encouraging patients to have blocks loosened and improving the diagonal pattern of movement for walking (gross motor control), work on the two separate halves of the body / work on organization of the two hemispheres, massage of the fingertips and fine motor control exercises, - behaviour therapy measures, empathizing with the patient, encouraging the patient to accept hitherto repressed peculiarities and to become desensitized to them, passing on any relevant expert advice available,(with a view to tackling the problem currently at issue), - work on factual themes, desensitizing the patient to school-based tasks, engaging the support of the school, - tackling nutritional issues / problems with the digestive system, - seeking the cooperation of others in helping to avoid actions that may have a harmful effect (e.g. changing the position of the patient in the case of Louis Bar syndrome). Monitoring and documenting heart rate and blood oxygen level readings gave some clue as to how effective the measures taken were. The question as to why this testing instrument has never found its way into the therapy room is one that cannot be answered. A good reliable instrument is not exactly cheap, but they are durable. Perhaps the dubious nature and the unreliability of lie detectors have also contributed to a reluctance to use them; the situation here, however, is quite different in as much as it is the patient that has a keen interest in the progress being made. Maybe it is an instrument unknown to practising therapists or one they are merely unaccustomed to using. However, the fact that they have been in use among paediatricians for some time is an indication of their usefulness. They are certainly to be recommended. Unfortunately, such an instrument cannot provide detailed information on peculiarities rooted in one or other of the two hemispheres; this might be something worth pursuing in the future. The findings of a further analysis of the previously collected data mentioned above are presented in the appendix below; the results are intended to give a "behind the scenes" insight into what originally prompted the use of the instrument. Information on the recording of the data used or any other preliminary information required can be obtained by referring to the article concerned. Appendix Changes in heart beat rates in babies upwards of 4 months The entire procedure (measurement of HR during the treatment of babies) can be divided into three phases: the time prior to treatment (=waiting phase / readings 1 and 2), during the treatment itself (=treatment phase, readings 2 and 3 immediately before and after treatment respectively) and some time after treatment (post-treatment phase readings 3 and 4), making a total of 4 readings (1st, 2nd, 3rd, 4th reading) covering the three phases. The values of the 3rd reading catch the eye in as much as that although they still correlate to a highly significant degree with the values of the other 3 readings, they correlate with these on a much lower level (.44 to .32) than the others correlate with one another (.84 to .71). By establishing the differences between the various readings (the difference in HR / waiting phase, the difference in HR / treatment phase, the difference in HR / post-treatment phase), changes in HR at each stage can be ascertained. There are already quite substantial differences in HR to be seen in the 1st reading. If these HR readings are then set in relation to changes in HR in the waiting phase using cross-table methods, we get the following picture: 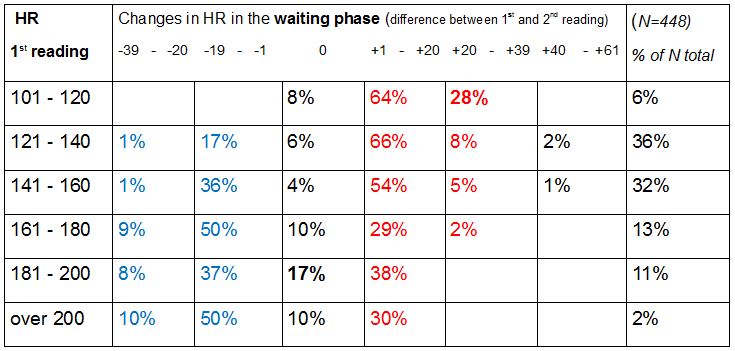 Table 1: Distribution of children according to changes in HR between the initial recording in the left-hand column and the second reading in the waiting phase; the percentage figure applies to babies beyond the age of 4 months. Method: Crosstabs (PSPP). The distribution is to a highly significant degree more than coincidental (Pearson Chi squared sign. 2-sided .000 df =20, N=448); blue signifies a fall in HR, red an increase in HR. Particularly noteworthy figures are shown in bold. The figures in each line of this and other tables should add up to 100%; any slight deviation one way or the other is due to the rounding-off process. The following can be seen from the results shown in Table 1: 1. Almost all the babies that had a particularly low initial HR reading on their arrival (101 - 120) tended to experience an increase in HR. 2. Of those babies that had a high initial HR reading of between 180 and 200, the HR of more than a third showed a tendency to fall. 3. Most of the babies with a medium initial HR reading (141 – 160) experienced only slight changes in HR. As one might expect, the treatment phase induced changes in HR, but a comparison of the second and third readings also revealed a much wider range of deviation. It is particularly noticeable that a relatively large number of the babies that had a high HR immediately prior to treatment (2nd reading) retained their high HR level during the treatment phase (20%) unlike and in contrast to the babies in the group with noticeably low HR (2nd reading), who all exhibited a change in HR. Taking the groups with frequencies of under 180 as a whole, there were more falls in HR during the treatment phase (by comparison to the second reading) than increases (exception: babies with HR 121 – 140); these falls are most apparent (75% in all) in the group of babies that had a low HR immediately prior to treatment. It is the babies with low HR that begin to catch the eye in Table 1. A different picture again is seen in the post-treatment phase: here, too, in the group of babies with a higher initial HR (181 – 200 in the 3rd reading) the proportion of babies with a stable HR level (13%) is greater than in the other groups. With few exceptions babies with an initially lower HR exhibit a higher HR in the post-treatment phase, the rise all the more pronounced the lower the rates recorded in the third reading (this is shown by the high degree of correlation of -.77 between the HR measured in the third reading and the differences measured in the fourth reading (Pearson, 2-sided, sign. .000). Table 3 (post-treatment phase) shows increases in HR to be more prevalent than decreases in all the sub-groups. Courses in stable sub-groups It was these different patterns noticed previously in the course of events that actually led to this statistical study. To make it easier to follow the course of events 3 sub-groups (=groups) will now be selected from the 1st HR reading (with a fixed frame of reference); the changes / differences in HR will then be observed in each of the three phases. The composition of each group therefore remains the same throughout. For selection purposes: the groups had to be represented in all measurements and must have been conspicuous in some way; "runaways" and "extreme cases" are avoided as far as possible. Group 1: he group of babies with a HR of 100 – 120 in the first reading (figures shown on a yellow background in the tables). Babies with these heart rates had attracted attention by exhibiting an increase in HR during the waiting phase, more frequent and more substantial decreases in HR during the treatment phase, and by showing quite pronounced increases in HR in the post-treatment phase. Group 2: the group of babies with a HR of 141 - 160 in the first reading. In the case of these babies with medium HR readings changes in heart rate appeared to vary only moderately (figures shown on a grey background in the tables). Group 3:the group of babies with a HR of 181 – 200 in the first measurement. These babies attracted attention on account of their fast heartbeat when HR was first measured. Contrary to (initial!) expectations, however, the stability values (within the 0 % tolerance) of these babies were the highest throughout all 4 phases (figures shown on a green background in the tables). Mean value 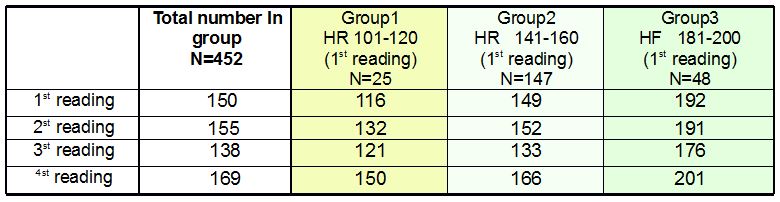 Table 2: HR mean values in the group as a whole and in the 3 sub-groups in the 4 measurements The mean values (MW) in Table 2 already show a clear trend. All the mean values differ highly significantly from one another, with one exception: the mean values in the third readings of groups 1 and 2 do not differ significantly. On the one hand it is important because it is the measurement taken immediately after the treatment, but, on the other hand, caution must prevail when evaluating this circumstance due to the fact that the initial HR readings are not taken into account. Distribution Table 3 below is an attempt to get a better grasp of the differences between the groups. The figures show the course of changes in HR in the three phases. For each of the three phases there are percentage figures that denote the distribution of babies (within their own particular group) according to the corresponding changes in HR. Minor deviations of up to -19 to + 20 have been classed together and combined for the sake of clarity. 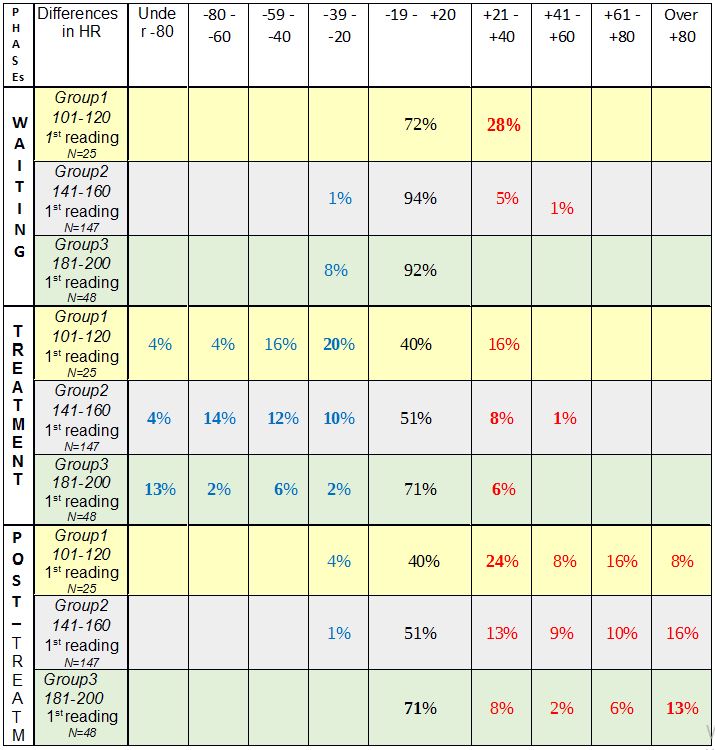 Table 3: Percentage distribution of babies according to the extent of changes in HR in all three groups in the WAITING phase, TREATMENT phase and POST- treatment phase. The composition of the three groups selected after the first reading remains the same throughout Table 3. The figures have been rounded off and add up to 100% in each group. All differences in the distribution of the babies according to the differences in HR (see the direction and extent of change quantified at the top of each column) in the three groups and in all three phases are over-coincidental to a highly significant degree. The larger proportion of babies with an increase in HR in the waiting phase in group 1 (an increase in HR of over 20 beats per minute in 28% of cases) was already mentioned above (see Table 1). One should bear in mind, however, that this still leaves the remaining 72% of babies in this group retaining their relatively low HR reading and that it is in this very same group that the proportion of babies exhibiting a further decrease in HR in the treatment phase (44% compared with 40% and 23% in the other two groups) is high. A decrease in HR among babies that already exhibited a low HR was not only found to be more frequent and more substantial here in Table 3, but in babies in the group as a whole in the treatment phase. In the post-treatment phase it is once again group 3 that records the most babies with stable readings (69%). Intensity of HR deviation The sum total of the absolute values of the 3 differences (waiting phase, treatment phase, post-treatment phase) can provide some information as to the intensity of HR fluctuations. If cross-tabling is used to set this sum in relation to affiliation to the three groups, the resulting distribution is more than coincidental to a significant degree. 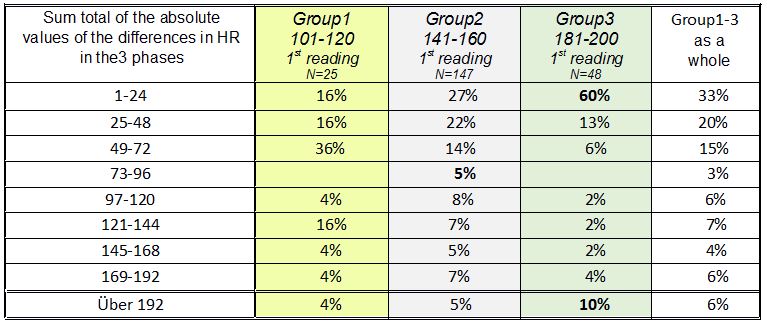 Table 4: Distribution of the recoded sums of absolute values of changes/differences in HR in the 3 phases according to their affiliation to groups 1 – 3 - What is immediately noticeable is how poorly the absolute values 73 – 96 are represented. - Equally striking is the fact that 10% of the babies with initially high HR bucked the trend in the rest of group 3 by showing quite appreciable fluctuations. Recourse to test subject numbers revealed that these were the babies in this group that had particularly high readings in the post-treatment phase and particularly low ones in the treatment phase. Age may have played a part in the case of some of these babies (4 months) that could be seen as belonging more to the group of babies that were omitted from this data analysis (1 – 3 months old), but this does not apply in all cases. In mean value terms the babies in group 3 are one month older than those in group 2 but they share practically the same MV in terms of age as the babies in group 1. Synopsis The results show that in Group 1, the group of babies with low initial HR readings, there were more babies with greater fluctuations in each of the three phases, exhibiting bradycardic (treatment phase) as well as tachycardic (waiting phase and post-treatment phase) reactions. With the babies that had high initial HR readings (Group 3) the opposite was the case; here there were fewer babies in the groups exhibiting greater deviations, with the exception, however, of the 10 – 13% of babies where quite considerable differences in HR were recorded. The statistical analysis of the data presented here provides no help towards offering any explanation of possible underlying causes. The age factor, which was the reason why the very young babies were not included in this data analysis in the first place, but which was expected to be an issue, played no major role in the results obtained (apart from those babies in Group 3 referred to above). The higher incidence of C2L in Group 1 (24%, twice as high as in the other two groups with 13% and 10%), though not statistically verified, is an observation that could be followed up in further studies or by practising therapists. The double displacement to the left which had been observed previously in the pilot study does not come to the fore in this data analysis, but the previous study involved a different set of test subjects, older children, and too little is known about the processes in between to allow any judgement to be made. Just as little is known of the conditions prevailing prior to arrival at the surgery and if the babies had the same HR under "normal circumstances" as they had here. It can justifiably be taken for granted, however, that the babies with low HR readings exhibited more marked differences in HR in all stages supposedly on account of the greater amount of energy required for the purpose of regeneration. Nevertheless, the findings raise more questions than they provide answers. Firstly, to what extent the test subjects selected (babies diagnosed with KISS in need of manual therapy treatment) has a restrictive bearing on the results. Analysis revealed no over-coincidental distribution of specific problems in the occipital region among the three sub-groups (apart from the greater incidence observed in the case of CL2). One positive factor is that the babies were free from infections as they would not otherwise have been treated. The question as to whether it could really be the case that pending events may cause a particularly low HR to fall even further would need to be followed up in further investigations. The connection between blood oxygen saturation level in a growing child in general and its level during the course of acquiring the knowledge and learning the civilizational skills so important in our lives, is one that is hardly likely to be disputed. One would therefore be well advised to pay greater general and professional attention to the occurrences described here and to take them into account when evaluating an individual´s peformance. The above-mentioned experience gathered in the therapy room (which prompted this discourse) is a warning reminder that greater attention should be paid, in all manner of ways, to so-called "basic" processes. Put quite bluntly: The "working basics" make a much bigger contribution to cognitive performance than we realize, and must be fully functioning. How can a child be expected to learn to read quickly when turning its eyes to focus on the printed word causes its HR to fall to little more than 20, which is then followed by a long stabilization phase, during which the syllables it has just been learning are forgotten? Much credit must go to Dr. Zelinsky, albeit in a slightly different connection, for pointing out the need to devote greater attention to what are falsely considered to be “simple“, primitive processes, and to where their centres of energy are concentrated. LLinas also opens up new perspectives on things with his example of the "captain" and "crew" working hand in hand. The underlying causes of the phenomena observed here in the case of children with a particularly low HR may stem from many quite different sources: currently active or long-standing ones, singular or cumulative ones. In the case of older children it should be taken into account that a fall in HR can result in a poorer supply of blood to the periphery, which may hinder fine motor systems currently active (one becomes aware of this upon noticing that the supply of blood to the all-important fingertips is no longer sufficient to allow the instrument to function properly). A reduced supply of blood to the periphery could also cause systems such as approach (=touch) to withdraw and allow avoidance to dominate (see the well-known game involving activation and inhibition of systems located in the left and in the right hemisphere of the brain respectively). Such processes may quite easily hide a child´s real potential. As it is the ultimate aim of diagnosis, however, to lead beyond random chance and to know more about and to gain a greater understanding of a particular problem, one would be well advised to have a closer look at functional connections not visible from the outside. It was this realization 20 years ago that has led to the continued use of this instrument in the diagnosis and therapy of developmental disorders to this day; the information given by patients is set in relation to the HR recording, which, it is hoped, will help in the search to find the causes. Copyright 2019 Dr. Sigrid Graumann-Brunt |

